Loyalty in the U.S. Health Insurance
Executive Summary
Loyalty and wellness reward programs have become a central pillar of competitive differentiation in the U.S. health insurance market. What began as simple incentive structures to encourage annual wellness visits has evolved into sophisticated digital ecosystems that tie member behavior, clinical outcomes, and plan economics together in a single platform.
This white paper examines the strategic rationale, program mechanics, and comparative positioning of loyalty programs offered by the three dominant national carriers — Humana (Go365), UnitedHealthcare (UHC Rewards / Rally / Motion), and Cigna (Take Control Rewards / Healthy Rewards). These programs span both commercial employer-sponsored insurance and Medicare Advantage markets, and collectively reach tens of millions of Americans.
Key findings from this analysis include:
All three programs offer up to approximately $300–$400 in annual member rewards, anchored to preventive care, health assessments, and activity participation.
UnitedHealthcare commands the greatest scale, while Humana leads on clinical integration and documented ROI, and Cigna differentiates through a hybrid financial model combining points-based rewards with direct partner discounts.
Highly engaged members show measurably better health outcomes — including significantly fewer emergency room visits and hospital admissions — making these programs strategically valuable for plan economics, not just member retention.
The integration of wearables, behavioral data, and personalization technology is accelerating, and programs that fail to invest in digital UX risk member disengagement.
1. Introduction: Why Loyalty Programs Matter in Health Insurance
The U.S. health insurance market is undergoing profound transformation. Rising medical costs, a wave of chronic disease, intensifying competition for Medicare Advantage enrollees, and growing consumer expectations around personalization are reshaping how plans compete for and retain members.
Against this backdrop, loyalty and wellness reward programs have emerged as a multi-purpose strategic tool. They serve simultaneously as a member engagement mechanism, a clinical intervention, a retention driver, and a brand differentiator. Employer-sponsored plans now cover approximately 154 million Americans, and the Medicare Advantage market continues to expand as the population ages — both represent fertile ground for these programs.
The average annual health insurance premium reached $8,435 for single coverage and $23,968 for family coverage in 2024, with premiums increasing roughly 7% year-over-year. In an environment where cost is the top reason Americans skip care, plans that can demonstrably help members navigate their health — while rewarding them for doing so — hold a significant competitive advantage.
Unlike loyalty programs in retail, where the primary objective is frequency of purchase, health insurance loyalty programs are explicitly designed to change behavior in ways that benefit both the member and the insurer. Preventive care utilization, chronic disease management, and reduction of costly acute episodes are the metrics that matter — and the programs reviewed in this paper are built around precisely these outcomes.
2. Market Context: The U.S. Health Insurance Landscape
2.1 Commercial and Medicare Advantage Segments
Health insurance in the United States is broadly divided into employer-sponsored commercial plans, individual market plans (including ACA Marketplace offerings), and government programs (Medicare, Medicaid). Loyalty programs are most prevalent in the commercial employer group market and in Medicare Advantage (MA).
Medicare Advantage is particularly significant for this analysis. MA plans are offered by private insurers as an alternative to traditional Medicare, and they compete aggressively on supplemental benefits — including wellness programs, dental, vision, and gym memberships — that go beyond what original Medicare covers. As of 2025, ACA Marketplace enrollment reached a record 24 million consumers, and Medicare Advantage membership continues to grow as the boomer generation ages into eligibility.
ACA Marketplace enrollment has reached a record high of 24 million consumers in 2025, contributing to some of the lowest uninsured rates in U.S. history. The three national carriers profiled in this paper — UnitedHealthcare, Humana, and Cigna — operate across all of these market segments, though their strategic emphasis differs.
2.2 Why Loyalty Programs Are a Strategic Priority
Member experience has become a direct driver of plan retention and employer purchasing decisions. According to J.D. Power's 2025 U.S. Commercial Member Health Plan Study, the national average satisfaction score among commercial health plan members is 563 out of 1,000, but scores vary dramatically across regions and carriers. Leading plans are differentiating through digital convenience, clarity of communication, and member-first design — precisely the attributes that well-designed loyalty programs deliver.
A notable 20% of employers cite low employee satisfaction with their health plan as a factor in plan-switching decisions. For plans competing in the large employer market, this makes the member experience of reward programs a commercially significant variable.
Beyond retention, loyalty programs address a clinical and economic priority. Chronic disease — particularly cancer, cardiovascular disease, diabetes, and obesity — remains the top cost driver for employer health plans. Programs that successfully increase preventive screenings, activity levels, and health assessment completion rates contribute directly to the plan's medical loss ratio and long-term population health performance.
3. The Three Leading Programs: A Comparative Analysis
3.1 Humana Go365
Program Overview
Go365 is Humana's flagship wellness and rewards platform, serving members across Medicare Advantage, employer-sponsored commercial plans, and individual plan segments. The program operates on a gamified points-based architecture, in which members accumulate points by completing health-promoting activities and advance through status tiers — Blue, Bronze, Silver, Gold, and Platinum — unlocking progressively greater rewards.
How Members Earn
Members earn points through a wide range of activities, including: completing health risk assessments; obtaining preventive screenings (mammograms, colorectal cancer screenings, flu shots); logging verified fitness activities; participating in disease and care management programs; engaging in social or community activities; and completing educational health modules. The program is accessible via a dedicated mobile app that integrates with major fitness trackers and wearable devices.
Reward Structure
Points are redeemable in the Go365 Mall for gift cards to major retailers (including Walmart and Shell), health-related merchandise, and, in certain plan designs, premium reductions. Rewards have no cash value and must be earned and redeemed within the same plan year. Maximum annual reward value can reach $300 or more depending on engagement level and plan design.
Target Markets
Go365 is available to Humana members across Medicare Advantage plans, fully insured commercial employer plans, and — through the Humana Healthy Horizons brand — Medicaid managed care programs in select states. This cross-segment reach makes Go365 one of the most versatile platforms in the market.
Documented Outcomes
Humana has published the most robust clinical and financial outcome data of the three carriers reviewed here. A five-year internal study of approximately 10,000 Humana employees enrolled in Go365 found significant improvements in health behaviors: the share of participants exercising 150 or more minutes per week nearly doubled, rising from 36% to 62% by year five. Fruit and vegetable consumption also increased substantially over the same period.
Most significantly from an economic standpoint, highly engaged members spent on average $116 less per month on healthcare compared to low-engaged members by year five. These members also experienced 35% fewer emergency room visits and 30% fewer hospital admissions — a finding with direct implications for plan medical costs.
A broader multi-employer study of approximately 135,000 fully insured employees confirmed that as engagement in Go365 increased over four years, claims experience improved, health satisfaction rose, and healthcare utilization patterns shifted favorably. This evidence base provides strong justification for Go365's continued investment and positions Humana as the leader in demonstrable ROI among the programs reviewed.
Key Differentiators
Go365's primary differentiators are its gamified tier structure (which creates ongoing engagement incentives), its deep integration with clinical care management programs, and its multi-segment availability spanning Medicare, commercial, and Medicaid. The program's documented ROI makes it particularly compelling in employer group sales cycles where benefit committees demand evidence of value.
3.2 UnitedHealthcare — UHC Rewards / Rally / Motion
Program Overview
UnitedHealthcare's wellness and loyalty ecosystem is the most expansive in the U.S. market by reach, serving tens of millions of members across commercial, Medicare Advantage, and employer group segments. The platform has evolved through the integration of multiple products: Rally (a digital wellness and engagement platform), UHC Rewards (the incentive layer), and Motion (an activity-based reward program tied to step-counting via wearables). Together, these tools form an integrated digital suite that goes well beyond simple points redemption.
How Members Earn
Members earn rewards through multiple pathways: completing health surveys and assessments, achieving step-count or activity goals tracked via wearables and smartphones, obtaining preventive health screenings, participating in mission-based health challenges, and engaging with personalized health content. The UHC Rewards platform is designed around behavioral science principles, using personalized nudges and goal-setting frameworks to sustain ongoing engagement.
Reward Structure
Rewards can take the form of cash-equivalent incentives, gift cards, and premium credits — with maximum annual values reaching $300–$400 depending on the specific plan design. The program's integration with employer benefit portals enables seamless single-sign-on access, reducing friction in the reward redemption experience.
Target Markets
UHC's platform is available across the full commercial employer market and Medicare Advantage, making it the broadest-reaching program in this analysis. UnitedHealthcare covers over 50 million Americans in total, and its wellness platform benefits from this massive installed membership base.
Reported Outcomes
UnitedHealthcare has reported high participation rates and documented measurable improvements in health behaviors among enrolled members. The scale of the platform also enables richer population-level analytics that can inform care management and plan design decisions. Integration with clinical data — including screening reminder systems and care gap identification — makes the UHC platform more than a consumer reward program; it functions as a clinical engagement infrastructure.
Key Differentiators
UHC's dominant differentiators are scale and personalization technology. The Rally platform enables a highly individualized digital experience, presenting members with targeted health missions and content based on their health status and prior behavior. The integration with wearable devices and the behavioral nudge architecture are among the most sophisticated in the industry. For large national employers seeking a single platform across diverse employee populations, UHC's depth of digital infrastructure is difficult to match.
3.3 Cigna — Take Control Rewards / Healthy Rewards
Program Overview
Cigna's loyalty offering combines two distinct value mechanisms: a points-based reward system (Take Control Rewards) through which members earn points for preventive care and wellness activities, and a partner discount program (Healthy Rewards) that provides ongoing savings on health-related products and services. This dual-model approach distinguishes Cigna from its peers by offering both aspirational accumulation rewards and immediate transactional savings.
How Members Earn
Members earn points by completing preventive care visits, health risk assessments, participation in disease management programs, fitness challenges, and other wellness activities. Points can be converted into prepaid Visa cards or health-item allowances, with an estimated maximum annual value of approximately $325 per member. The Healthy Rewards component offers discounts on gym memberships, fitness equipment, weight management programs, and vision and hearing services through a network of national partners.
Target Markets
Cigna's programs serve commercial employer group plans and Medicare Advantage members. Cigna (now part of The Cigna Group, following the Evernorth integration) has a significant presence in the employer health benefit market and has been investing in integrated care delivery models that complement its wellness incentive programs.
Reported Outcomes
Cigna reports increased preventive service utilization and improved perceived plan value among members participating in its wellness programs. While Cigna's published outcome data is less granular than Humana's Go365 studies, the carrier's emphasis on preventive care aligns with its broader strategy of managing chronic disease costs — cancer, cardiovascular disease, and diabetes remain the top cost drivers for employer health plans, and Cigna has invested in guided, personalized approaches to chronic condition management.
Key Differentiators
Cigna's primary differentiators are the flexibility of its hybrid value model and its strong marketing positioning. The combination of points-based rewards with an always-on discount network means that members receive tangible financial value from day one of enrollment, without needing to accumulate points before realizing benefit. The Healthy Rewards discount network also creates a persistent touchpoint between the member and the plan, reinforcing the perception of plan value beyond the clinical interaction.
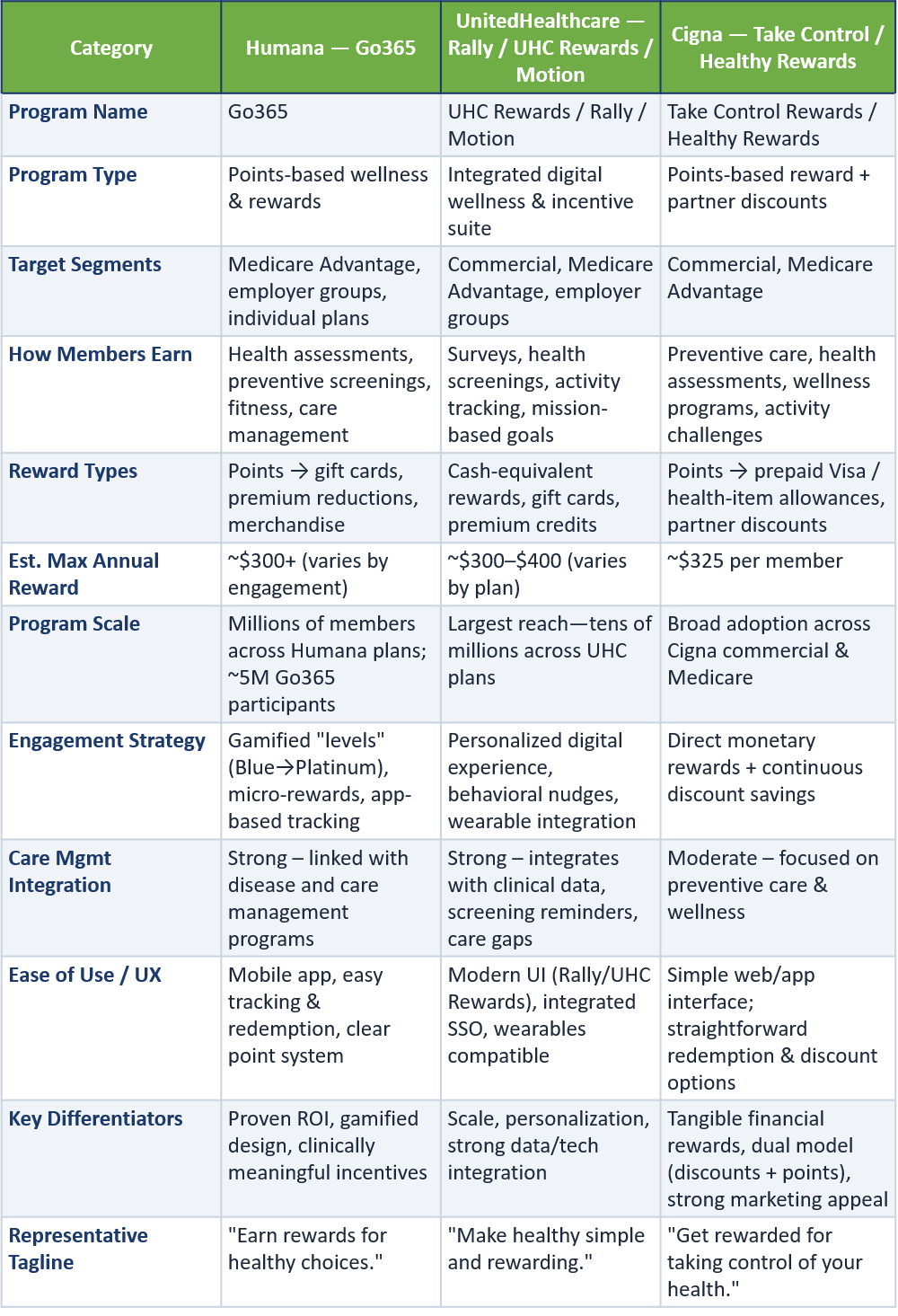
4. Head-to-Head Comparison
The following table provides a structured comparison of the three programs across key dimensions, based on publicly available program information as of November 2025.
5. Strategic Implications
5.1 For Health Plans
The three programs reviewed represent different strategic bets on how to drive member engagement and clinical value. Plans considering the design or enhancement of their own loyalty program should evaluate the following strategic dimensions:
Clinical integration depth: Programs tightly linked to care management, care gap identification, and preventive screening reminders generate superior health outcomes and plan economics. Humana's Go365 model — where wellness activities are connected to disease management programs — provides a template for maximizing clinical ROI.
Personalization and digital experience: Members increasingly expect the same level of personalization they receive from consumer platforms like Netflix or Amazon. UHC's Rally platform exemplifies how behavioral data and machine learning can deliver targeted health missions and sustained engagement. Plans that invest in this capability will have a structural advantage in member retention.
Reward model design: The choice between a pure points model, a cash-equivalent model, or a hybrid discount model carries different implications for engagement patterns, redemption economics, and member perception. Cigna's hybrid model reduces the barrier to perceived value, while Humana's tier-based gamification creates ongoing motivation for deeper engagement.
Segment-specific design: Medicare Advantage members have different engagement preferences and health needs than commercial employer group members. Programs designed for multiple segments should tailor the activity types, reward values, and UX appropriately for each population.
5.2 For Employers
For HR and benefits leaders evaluating health plan options, loyalty and wellness program quality has become an increasingly important criterion alongside premium pricing, network breadth, and clinical quality ratings. Key questions to ask include:
What evidence does the carrier provide for health and cost outcomes among program participants — and at what level of statistical rigor?
How does the program integrate with the employer's existing wellness investments, EAP programs, and HR technology stack?
What is the realistic expected engagement rate among your employee population, and what does the carrier offer to drive initial activation?
For employers with a demographically diverse workforce, does the program offer meaningful activities and rewards for populations across all age groups and health statuses?
5.3 For Medicare Advantage Members
For Medicare beneficiaries choosing between Advantage plans, the quality and generosity of wellness reward programs can represent meaningful financial and health value. When comparing programs:
Assess the maximum annual reward value in the context of the plan's overall premium and cost-sharing structure.
Evaluate whether the rewardable activities align with your own health needs and habits — a program with generous rewards for gym attendance is less valuable to a member who prefers walking or home exercise.
Consider the ease of the app or web interface, particularly if technology comfort is a factor.
Understand what happens to unclaimed rewards — all three programs reviewed require redemption within the same plan year, meaning unredeemed points are forfeited.
6. Regulatory Considerations
Wellness incentive programs in health insurance are subject to a layered regulatory framework. Under the Affordable Care Act and its implementing regulations, outcome-based wellness programs in employer-sponsored group health plans may offer incentives of up to 30% of the cost of employee-only coverage (50% for tobacco-related programs), provided they meet requirements for reasonableness, alternative standards, and annual disclosure.
For Medicare Advantage plans, CMS regulates supplemental benefits — including reward and incentive programs — and has permitted plans to offer health-related supplemental benefits including rewards for completing healthy behaviors. Plans must ensure that reward structures do not constitute improper inducements to enroll, and gift cards or prepaid cards used for rewards cannot be used to purchase items covered by Medicare, Medicaid, or other federal programs, nor can they be converted to cash.
The EEOC has also issued guidance on wellness programs under the Americans with Disabilities Act (ADA) and the Genetic Information Nondiscrimination Act (GINA), though the regulatory landscape in this area has evolved over time. Plans and employers should ensure their wellness programs are designed to be voluntary and accessible to all eligible participants, including those with disabilities.
As these programs become more data-intensive — integrating wearable biometric data, health records, and behavioral analytics — privacy and data governance considerations are also increasingly salient. Plans should ensure that wellness program data collection and use complies with applicable state and federal privacy frameworks.
7. Future Outlook
The next generation of health insurance loyalty programs is likely to be shaped by several converging forces:
7.1 Wearables and Continuous Monitoring
The share of U.S. consumers using connected monitoring devices and digital health tools reached 43% in 2024, up from 34% in 2022. As wearable adoption continues to grow — particularly among younger commercial plan members — programs that can seamlessly integrate real-time biometric and activity data will be better positioned to offer continuous, personalized incentives rather than episodic reward events.
7.2 GLP-1 Medications and Chronic Disease Management
The rapid uptake of GLP-1 medications for obesity, diabetes, and cardiovascular conditions is creating a new dimension for wellness programs. Plans that successfully integrate chronic disease management support — including coaching, behavioral support, and medication adherence tracking — into their reward frameworks will be better positioned to manage the population health and cost implications of this pharmacological shift.
7.3 AI-Driven Personalization
Machine learning and AI are beginning to transform how wellness programs identify at-risk members, deliver personalized health recommendations, and predict which interventions are most likely to change behavior for a given individual. Carriers with large data assets and digital infrastructure — particularly UnitedHealthcare — are best positioned to capitalize on this capability in the near term.
7.4 Mental Health Integration
Mental health has become a central concern for employer plan sponsors, with survey data consistently showing high demand for mental health benefits. Only 50% of insurers currently cover mental health screenings despite employee demand. Loyalty programs that expand to include mental health check-ins, digital CBT programs, and stress management activities will address a significant unmet need and open new engagement pathways.
7.5 Value-Based Care Alignment
As health insurers increasingly participate in value-based care arrangements with providers, loyalty programs have the potential to serve as a demand-side complement to supply-side quality initiatives. Programs that reward members for choosing high-value providers, completing post-discharge follow-up care, or engaging in shared decision-making will deepen the alignment between member behavior and the goals of value-based contracts.
8. Conclusion
Loyalty and wellness reward programs have moved from a niche benefit enhancement to a core strategic asset in U.S. health insurance. The three programs reviewed in this paper — Humana Go365, UHC Rewards / Rally / Motion, and Cigna Take Control Rewards / Healthy Rewards — each represent a distinct strategic approach to the common goal of engaging members in their own health.
Humana leads on the depth of clinical evidence and the strength of integration between wellness incentives and disease management. UnitedHealthcare commands unmatched scale and has built the most sophisticated digital personalization infrastructure. Cigna differentiates through a hybrid financial value model that delivers immediate savings alongside aspirational point rewards.
For plans, employers, and benefits advisors, the strategic lesson is clear: wellness loyalty programs, when thoughtfully designed and rigorously measured, are not a cost center but an investment with documented returns in member health, plan economics, and competitive positioning. The carriers that build the deepest, most clinically integrated, and most personalized programs will be the ones best equipped to compete for — and retain — members in an increasingly demanding market.
Sources & References
Primary Source
Aramis Advisors LLC. Healthcare Loyalty Program Comparison (internal comparative analysis, November 2025). www.aramisllc.com
Industry & Market Research
Deloitte Insights. 2025 U.S. Health Care Executive Outlook. Deloitte LLP, December 2024.
J.D. Power. 2025 U.S. Commercial Member Health Plan Study. J.D. Power, April 2025.
Mercer Marsh Benefits. Health Trends 2026: Key Trends Shaping Employer-Provided Health Benefits. Mercer, 2025.
Aon. Key Trends in U.S. Benefits for 2025 and Beyond. Aon plc, 2025.
McKinsey & Company / BEInsure. 2025 U.S. Health Insurance Market Trends. 2025.
Program Documentation
Humana Inc. Go365 Wellness & Rewards Program Overview. www.go365.com / www.humana.com. Accessed 2025.
Humana Inc. Go365 Fully Insured Outcomes Study (135,000 member multi-employer study). Published case study, go365.com.
Fierce Healthcare. 'Humana Sees Promising Results in 5-Year Study of Go365 Wellness Program.' August 2019.
Chapman Institute. 'Humana Wellness Program Evaluation Study — GO365.' WellCert publication.
UnitedHealthcare. UHC Rewards / Rally / Motion Program Documentation. www.uhc.com. Accessed 2025.
Cigna Healthcare. Take Control Rewards / Healthy Rewards Program Documentation. www.cigna.com. Accessed 2025.
Regulatory & Policy Sources
Centers for Medicare & Medicaid Services (CMS). Medicare Advantage Supplemental Benefits Policy Guidance. cms.gov.
U.S. Department of Health & Human Services. ACA Wellness Program Regulations (29 CFR Part 2590). hhs.gov.
Healthcare Dive. 'Health Insurers Will Step Off the Roller Coaster in 2025.' January 2025.